Table of Contents
- What is Peripheral Artery Disease (PAD)?
- Who is Affected and What are the Main Risk Factors?
- Symptoms According to Disease Stages
- How is Leg Artery Blockage Diagnosed?
- When Does Treatment Become Mandatory?
- Current Treatment Methods for Leg Artery Blockage
- Conclusion: The Meaning Beyond Leg Pain
- Summary: Frequently Asked Questions
What is Peripheral Artery Disease (PAD)?
The clean blood pumped by the heart is distributed throughout the body via the main artery called the aorta. The arteries going to the legs are also part of this system. In the process of atherosclerosis (hardening of the arteries), excess cholesterol and fat particles in the bloodstream accumulate on the inner surface of the artery wall, forming structures called “plaques.” These plaques grow over time, narrowing the artery and preventing blood from flowing freely. This narrowing or complete blockage is called leg artery blockage.
Who is Affected and What are the Main Risk Factors?
PAD is common, especially in individuals over 50, and the risk increases with age. It is more frequently observed in men than in women. The most important risk factors that accelerate the development of the disease are:
- Smoking: It is the strongest and most preventable risk factor for PAD. Smoking directly damages the inner lining of the artery wall (endothelium), triggering plaque formation and increasing blood clotting tendency.
- Diabetes: Diabetes significantly accelerates the process of atherosclerosis and often affects smaller vessels, making treatment more challenging.
- High Blood Pressure (Hypertension): Continuously applies high pressure to the artery walls, causing them to lose elasticity and become damaged.
- High Cholesterol (Dyslipidemia): Especially high LDL (bad cholesterol) levels form the main building blocks of plaques.
- Chronic Kidney Failure: Increases calcification in the artery wall, paving the way for the disease.
- Genetic Predisposition: A family history of early-onset vascular disease increases the risk.
Symptoms According to Disease Stages
The symptoms of the disease vary depending on the degree and location of the blockage.
1. The Most Common Symptom: Pain While Walking (Claudication)
The most typical and early symptom of the disease is cramping pain, fatigue, or a feeling of tightness in the legs, especially in the calf muscles, after walking a certain distance. This pain is called claudication. Increased muscle activity during walking requires more oxygenated blood. However, the narrowed artery cannot meet this need, and pain occurs in the muscles. The pain completely subsides after the patient rests for a few minutes, but it reappears at the same distance when walking continues. This condition is also known as “window shopping disease” among the public because it causes patients to stop and rest frequently.
2. Advanced Stage Symptom: Rest Pain
As the disease progresses, blood flow decreases so much that the muscles cannot be adequately nourished even at rest. In this case, severe, burning pain begins in the feet and toes, especially at night when lying down. The patient feels the need to hang their leg off the bed to relieve the pain. The presence of rest pain indicates that the condition has become serious and the limb is at risk.
3. Final Stage: Critical Limb Ischemia and Ulcers
In untreated advanced cases, blood flow decreases to a level insufficient to sustain tissue viability. At this stage, non-healing wounds (arterial ulcers) appear on the foot, toes, or heel with even minor trauma or spontaneously. These wounds are extremely painful. If the process progresses further, tissue death (gangrene) starting from the toes becomes inevitable. This is an emergency situation that carries the risk of limb amputation.
How is Leg Artery Blockage Diagnosed?
Diagnosis is made by listening to the patient’s complaints, a detailed physical examination, and modern imaging methods.
- Physical Examination: The doctor manually checks the pulses in the foot (dorsalis pedis, posterior tibial). Absent or weak pulses are an important finding. Signs of nutritional deficiency such as pallor, coldness, and hair loss on the leg skin are also sought.
- Ankle-Brachial Index (ABI): This is the simplest, fastest, and most objective test for diagnosing leg artery blockage. Blood pressure measurements are taken from the ankle and arm and then ratioed. Normally, this ratio should be between 1.0 and 1.4. Values below 0.9 support the diagnosis of PAD.
- Color Doppler Ultrasonography: Uses sound waves to map the vessels, show blood flow, and clearly determine the location and degree of narrowing.
- CT or MR Angiography: Advanced imaging methods used to visualize the entire vascular network in three dimensions before treatment planning.
When Does Treatment Become Mandatory?
The presence of claudication (walking pain) is an important warning that the patient’s general vascular health is deteriorating. These patients also have an increased risk of heart attack and stroke. Treatment becomes mandatory, especially in the following situations:
- If the patient’s walking distance has shortened to the extent that it hinders daily life activities (going to the market, working, etc.),
- If rest pain has started,
- If non-healing ulcers or gangrene have developed on the foot.
Current Treatment Methods for Leg Artery Blockage
Treatment is personalized according to the stage of the disease. The goal is to alleviate symptoms, increase walking distance, and most importantly, prevent limb loss.
1. The Foundation of Treatment: Lifestyle and Exercise
This is the cornerstone of treatment, and the success of all other methods depends on it.
- Definite Smoking Cessation: No treatment can be successful in the long term without quitting smoking.
- Risk Factor Control: Blood pressure, cholesterol, and diabetes should be brought to ideal levels with medication.
- Supervised Exercise Programs: Walking programs lasting 30-45 minutes, at least 3-5 days a week, significantly reduce walking pain by promoting the development of new capillaries (collateral circulation) and enabling muscles to use oxygen more efficiently.
2. Medication
In all PAD patients, blood thinners (Aspirin, Clopidogrel) are routinely used to prevent clot formation and reduce the risk of heart attack, and cholesterol-lowering drugs (statins) are used to stabilize plaques. Additionally, special medications to increase walking distance may be prescribed by the physician.
3. Minimally Invasive (Endovascular) Treatments
In these methods, the narrowed or blocked vessel segment is typically opened from the inside by entering through a small needle in the groin artery, guided by angiography.
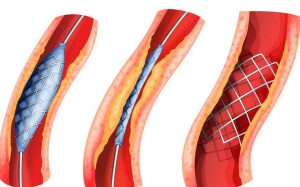
- Balloon Angioplasty: The narrowed area is expanded by inflating a special balloon.
- Stent Placement: A metal mesh (stent) is placed to prevent the vessel from re-narrowing after balloon expansion.
- Atherectomy: This is the process of scraping or shaving plaques inside the vessel with special devices.
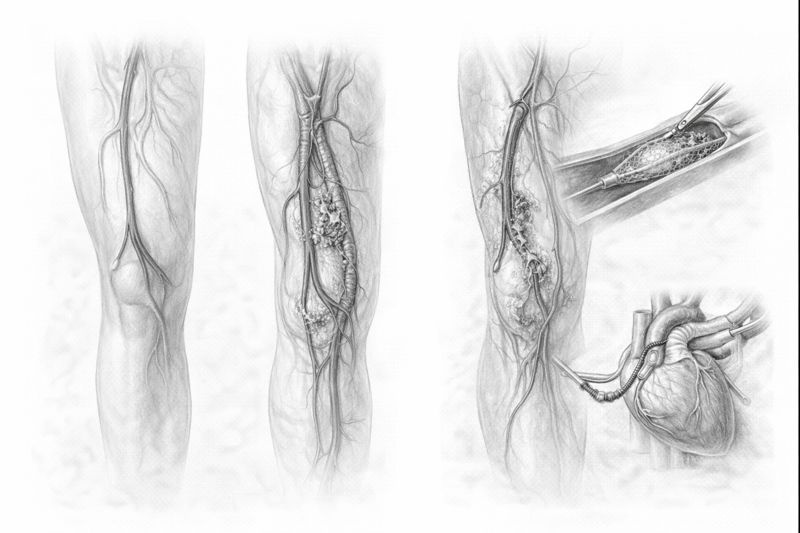
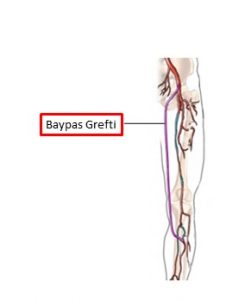
4. Surgical Treatment (Bypass Surgery)
This is preferred in cases where the blockage covers a very long segment, endovascular methods are unsuccessful, or critical limb ischemia (rest pain, ulcer) is present. In this surgery, a new pathway, a bypass, is created between the segment before and after the blockage, using a vein taken from the patient’s own leg or an artificial vessel. This allows blood to reach the foot by bypassing the blocked area.
Conclusion: The Meaning Beyond Leg Pain
Leg artery blockage is not just a condition that makes walking difficult, but an important indicator that the entire vascular system of the body is at risk. Leg pain that occurs during walking and subsides with rest should not be dismissed as “old age” or “fatigue.” Thanks to early diagnosis, control of risk factors, and modern treatment methods, it is possible to both improve quality of life and prevent serious consequences such as heart attack, stroke, and limb loss. If you are experiencing symptoms, it is vital to consult a cardiovascular surgeon without delay.
Curious About Leg Artery Blockage?
You can review our special page for detailed answers to all your questions about symptoms, diagnostic methods, treatment options, and the surgical process.
Summary: Frequently Asked Questions
What are the symptoms of leg artery blockage?
Does smoking cause leg artery blockage?
Is non-surgical treatment possible?
How is it diagnosed, is it painful?
Does leg artery blockage carry a life-threatening risk?