In this article, you will find a detailed overview of modern medicine’s approach to this significant problem, including the underlying causes of carotid artery blockage, its warning signs, and current treatment methods.
Table of Contents
What is Carotid Artery Blockage (Carotid Artery Disease)?
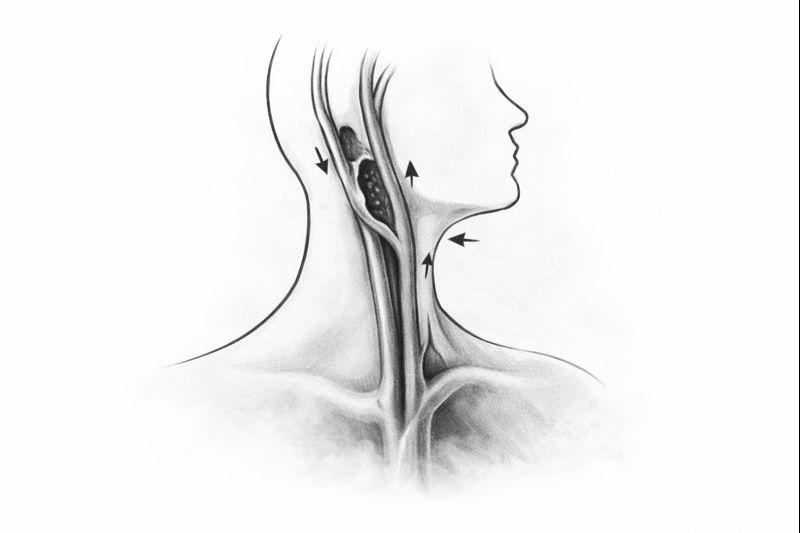
The carotid arteries, medically known as carotid arteries, are the main arteries that branch off the aorta (the main artery leaving the heart) and run on both sides of the neck, supplying blood to the anterior parts of the brain. A healthy artery wall is smooth and flexible. However, over time, especially in the presence of risk factors, a process called atherosclerosis, or “hardening of the arteries,” begins. In this process, cholesterol, fat, calcium, and other cellular waste products adhere to the inner surface of the artery wall, forming structures called “plaques.”
As these plaques grow, they progressively narrow the inner diameter of the artery and impede blood flow. This condition is called carotid artery blockage, or more accurately, carotid artery stenosis.
When the narrowing progresses, the risk of stroke arises through two main mechanisms:
- Reduced Blood Flow: When the narrowing reaches a critical level (80-90% or more), blood flow to the brain decreases so much that brain cells do not receive enough oxygen and begin to lose function.
- Embolism (Clot Formation): This is the more common and most dangerous mechanism. The surface of the plaque in the artery wall can crack over time. The body sends clot cells to the area to repair this crack. A small piece breaking off from this clot or the plaque itself can travel with the bloodstream and block a smaller artery in the brain, suddenly cutting off blood supply to that region and causing a stroke.
Who is Affected? What are the Risk Factors?
Carotid artery blockage typically occurs in individuals over 50 years of age, and its incidence increases with age. While it is more common in men, it is also a significant health concern for women in the post-menopausal period. The more risk factors present, the higher the likelihood of developing the disease:
- Smoking: The most important risk factor, directly damaging the inner lining of the artery wall (endothelium) and accelerating plaque formation.
- High blood pressure (hypertension): Constantly applies high pressure to the artery wall, disrupting its structure and triggering atherosclerosis.
- Diabetes: High blood sugar causes artery walls to lose elasticity and become more prone to plaque formation.
- High cholesterol levels: Especially LDL, known as “bad cholesterol,” is the main building block of plaques.
- Obesity and sedentary lifestyle: Trigger other risk factors (blood pressure, diabetes, cholesterol).
- Family history of vascular diseases: Genetic predisposition can lead to the disease appearing at an earlier age.
The most important point to remember is that atherosclerosis is a systemic disease. This means that a patient with carotid artery narrowing is highly likely to have similar problems in the coronary arteries (heart arteries) and peripheral arteries (leg arteries). Therefore, treatment should be planned with a holistic approach.
Symptoms of Carotid Artery Blockage: The Body’s Warning Signs
The disease often progresses insidiously and may not show any symptoms until the narrowing reaches 50-60%. When symptoms do appear, they are usually in the form of a Transient Ischemic Attack (TIA), which is a sign of a clot traveling to the brain. TIA is a precursor to a full stroke and requires urgent medical attention. These symptoms begin suddenly and usually resolve completely within a few minutes to a few hours:
- Temporary vision loss or blurred vision: Often in one eye, described as a curtain coming down and going up (Amaurosis Fugax).
- Numbness or weakness on one side of the body: Sudden loss of sensation or strength in the face, arm, or leg.
- Speech disturbance: Inability to pronounce words, slurred speech, or difficulty finding the right words.
- Facial asymmetry: Drooping or sagging on one side of the face.
- Dizziness and loss of balance: Especially important if accompanied by other symptoms.
- Temporary loss of consciousness or confusion.
Even if these symptoms completely disappear, it does not mean “there is no significant problem.” On the contrary, it is a warning period during which the risk of permanent stroke is highest within the first 24-48 hours.
How is Carotid Artery Blockage Diagnosed?
Early diagnosis is vital for preventing permanent and devastating consequences like stroke. Various methods are used for diagnosis, from simple examinations to advanced imaging technologies:
1. Physical Examination
An experienced physician may hear a “bruit” (a whooshing sound) when listening to the neck area with a stethoscope, caused by turbulent blood flow through a narrowed artery. This sound raises significant suspicion for carotid artery disease and requires further investigation.
2. Doppler Ultrasonography
This is the gold standard screening method for diagnosing carotid artery disease. Sound waves are used to measure the structure of the artery, plaques on its wall, and most importantly, the degree of narrowing and blood flow velocity. As it is a painless, harmless, and fast method, it is widely used for both screening and follow-up.
3. Advanced Imaging: Angiography Methods
These methods are used when critical narrowing is detected by Doppler ultrasound or when more detailed imaging is required for treatment planning.
- CT Angiography: A rapid method that creates three-dimensional images of the arteries by injecting contrast material.
- MR Angiography: A radiation-free alternative that images arteries using a magnetic field.
- Conventional Digital Angiography (DSA): The method that provides the clearest images, performed by inserting a catheter through the groin and directly injecting contrast material into the carotid artery. Since it is invasive, it is usually performed in the same session as stent treatment.
What are the Treatment Methods?
The treatment plan is determined with a multidisciplinary approach based on the degree of narrowing (in %), whether the patient is symptomatic or asymptomatic, their general health status, and age.
1. Medical Treatment and Lifestyle Management
This is the primary and fundamental treatment option for patients with a low degree of narrowing (below 50%) and no symptoms. The goal is to slow the progression of the disease and prevent clot formation.
- Blood thinners (Antiplatelets): Medications like aspirin or clopidogrel reduce the blood’s clotting ability, lowering the risk of embolism.
- Cholesterol-lowering drugs (Statins): Not only lower cholesterol but also stabilize plaque in the artery wall, reducing the risk of cracking and clot formation.
- Blood Pressure and Blood Sugar Control: Regular use of hypertension and diabetes medications is essential to protect the artery wall.
Lifestyle changes (quitting smoking, diet, exercise) are an integral part of this treatment.
2. Carotid Artery Stenting (CAS)
This is a minimally invasive procedure, usually performed by inserting a thin catheter through the femoral artery to reach the narrowed carotid artery area. After a filter (protective umbrella) is placed in the narrowed region to prevent clots from reaching the brain, the narrowed segment is expanded with a balloon, and a metal mesh (stent) is permanently placed to prevent the artery from re-narrowing. It is a good alternative for patients with high surgical risk (advanced age, severe heart or lung disease), those who have undergone previous neck surgery, or received radiation therapy.
3. Surgical Intervention (Carotid Endarterectomy – CEA)
This is the gold standard treatment method, especially for symptomatic patients who have experienced a transient ischemic attack or mild stroke within the last 6 months and have more than 50% narrowing in their artery. For asymptomatic patients, it is generally recommended if the narrowing is above 70-80%. In this operation, a small incision is made in the neck to access the carotid artery. The artery is temporarily clamped and opened, and the plaque inside is surgically scraped away. The artery is then closed, usually using a patch to widen it. It is a highly successful and permanent method with proven long-term results.
Is it Possible to Prevent Stroke?
Yes. Carotid artery blockage is not destiny, and preventing stroke is largely possible. If the disease is detected in time, risk factors are controlled, and appropriate treatment (medication, stent, or surgery) is applied, the risk of stroke can be reduced by 80-90%.
Steps to take for prevention include:
- Know Your Risks and Control Them: If you are in a high-risk group (smoking, diabetes, hypertension, etc.), undergo regular doctor check-ups and carotid artery Doppler ultrasonography without waiting for symptoms.
- Quit smoking immediately.
- Adopt a Mediterranean-style diet; avoid saturated fats and processed foods.
- Exercise at a moderate pace for at least 150 minutes per week (walking, swimming, etc.).
- Regularly use your medications to keep your blood pressure, cholesterol, and blood sugar levels within target ranges.
Conclusion
Carotid artery blockage is a silent but potentially devastating vascular disease that directly threatens the brain’s blood supply. Due to its often asymptomatic progression, proactive screening and regular check-ups are vital for individuals at risk. Early diagnosis and personalized treatment approaches offered by modern medicine can largely prevent permanent damage such as stroke. Never ignore warning signs from your body, such as temporary dizziness, speech disturbances, or vision loss, and seek medical attention immediately.
📌 Top 5 Questions
1. Is carotid artery surgery risky?
Like any surgical procedure, there are risks, but in experienced centers, this rate is around 1-2%. The risk of stroke caused by untreated severe narrowing is much higher than the risk of surgery.
2. Can artery blockage be opened with medication?
No, medications (blood thinners and statins) do not completely eliminate existing calcified plaque or open the artery like a drain cleaner. The role of medications is to stop plaque growth, prevent clotting on its surface, and reduce the risk of stroke.
3. Is stenting or surgery better?
This decision is made based on the patient’s age and artery structure. Generally, surgery (endarterectomy) is considered the “gold standard” and has better long-term results. However, stenting is a good alternative for patients with high surgical risk or those who have undergone previous neck surgery.
4. Can surgery be performed after a stroke?
Yes, but timing is crucial. It is generally recommended to intervene within the first 2 weeks after mild strokes (if there is no brain hemorrhage) to prevent a second and more severe stroke.
5. Which department should I go to?
For diagnosis and follow-up, you can consult Cardiovascular Surgery, Neurology, or Cardiology departments. If surgical intervention is required, you need to be evaluated by a Cardiovascular Surgery specialist.
Do You Have More Questions?
We have compiled the 25 most frequently asked questions and their detailed answers about carotid artery blockage, stroke risk, surgical process, and recovery period on a special page.
Summary Information
- Disease: Carotid artery blockage (carotid artery disease) is a serious vascular disease that develops due to atherosclerosis and increases the risk of stroke.
- Symptoms: Often insidious. Warning symptoms include dizziness, temporary vision loss, speech disturbance, and unilateral numbness and weakness.
- Risk Factors: Smoking, hypertension, diabetes, high cholesterol, obesity, and a sedentary lifestyle are the most important.
- Treatment: Treatment methods include medication, stenting (CAS), and surgery (Carotid Endarterectomy – CEA), depending on the degree of narrowing and symptoms.
- Prevention: The risk of stroke can be significantly reduced through a healthy lifestyle, effective management of risk factors, and regular doctor check-ups.