Table of Contents
Heart Valves and Their Function
The heart is a muscular organ that works tirelessly throughout life, pumping oxygenated blood to the body. During this pumping process, it is vital that blood flows in the correct direction and does not flow backward. The structures that ensure this “one-way flow” are the heart valves.
There are a total of four valves in the heart, each acting as a “gate”:
- Mitral Valve: Located between the left atrium and the left ventricle. It controls the flow of oxygenated blood from the lungs to the heart. It is one of the most frequently affected valves.
- Aortic Valve: Located between the left ventricle and the aorta, the body’s main artery. It is the final exit gate through which blood is pumped under pressure to the entire body.
- Tricuspid Valve: Located between the right atrium and the right ventricle. It regulates the flow of deoxygenated blood.
- Pulmonary Valve: Located between the right ventricle and the pulmonary artery. It ensures blood flows to the lungs for oxygenation.
In a healthy heart, these valves open completely with each heartbeat (allowing blood to pass) and close completely (preventing backflow). A malfunction in this mechanism increases the heart’s workload and eventually leads to fatigue of the heart muscle.
Causes of Heart Valve Diseases
Valve diseases are examined in two main groups based on the origin that causes damage to the valve structure.
Congenital Causes
In some individuals, the valve structure is abnormal from birth. The most common condition is a bicuspid aortic valve (Bicuspid Aorta), which should normally have three leaflets. Although this condition may not show symptoms in childhood, it can lead to calcification and stenosis after the age of 40-50, requiring treatment.
Acquired Causes
- Aging and Degeneration: As we age, calcification (hardening) and thickening can occur in the valves, similar to arteriosclerosis. This is the most common cause of aortic stenosis.
- Rheumatic Fever: Still prevalent in developing countries. Untreated beta-hemolytic streptococcal infections (strep throat) in childhood can lead to permanent damage, adhesions, and calcification in the valves years later.
- Mitral Valve Prolapse: This occurs when the valve tissue loses its elasticity, becomes loose, and bulges backward during closure. It can be genetically inherited.
- Heart Attack (Ischemia): Damage to the muscles supporting the valves during a heart attack can cause sudden, severe valve insufficiency.
- Infective Endocarditis: A serious infection caused by bacteria reaching the heart via the bloodstream and settling on the valves. It can perforate or damage the valve structure, requiring emergency surgery.
The Body’s Signals: Symptoms
Heart valve diseases can progress insidiously. The heart can tolerate an increased load for a long time; however, symptoms become apparent when its reserves are depleted. Pay attention to the following symptoms for early diagnosis:
- Shortness of Breath: The most common symptom. Initially, it may only occur when climbing stairs or uphill, but as the disease progresses, it can also be experienced when walking on flat ground or lying down at night (requiring more pillows).
- Easy Fatigue and Weakness: Muscles are deprived of oxygen because the body cannot pump enough blood.
- Palpitations (Arrhythmia): “Atrial Fibrillation” is common, especially in patients with mitral valve disease. It is the sensation of an irregular and rapid heartbeat.
- Chest Pain (Angina): Especially in aortic stenosis, chest pressure can occur due to impaired blood supply to the thickened heart muscle.
- Fainting (Syncope): A sudden decrease in blood flow to the brain can cause fainting or dizziness, especially during exertion (a symptom of severe aortic stenosis).
- Edema: If right heart failure develops, swelling occurs in the ankles and abdomen.
Common Valve Diseases
Valve disorders manifest mechanically in two ways:
[Image of heart valve stenosis vs regurgitation]
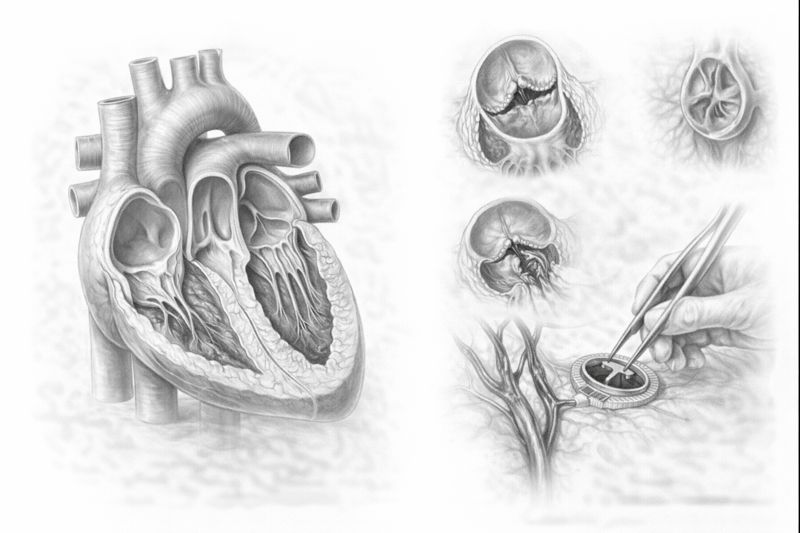
- Stenosis: The valve leaflets calcify or stick together, preventing them from opening fully. Blood flow becomes difficult, and the heart has to generate more pressure to pump blood. (e.g., Aortic Stenosis, Mitral Stenosis).
- Insufficiency (Regurgitation): The valve cannot close completely. Some of the pumped blood flows backward. The heart has to pump the same blood repeatedly, increasing its volume load and causing the heart to enlarge.
Diagnostic Methods
The first step in diagnosing the disease is a physical examination. Your doctor may hear a “murmur” sound caused by blood flowing through the faulty valve when listening to the heart with a stethoscope. The following methods are used for definitive diagnosis and grading:
- Echocardiography (ECHO): A heart ultrasound. It is the cornerstone of diagnosis. It shows the structure of the valves, the degree of stenosis or insufficiency, and the heart’s pumping strength.
- Transesophageal Echocardiography (TEE): Performed by swallowing a probe through the esophagus (similar to an endoscopy). It provides a much clearer image from the posterior vicinity of the heart. It is essential, especially for patients planning valve repair and for investigating blood clots.
- Cardiac Catheterization and Angiography: Can be performed before surgery to assess the condition of the coronary arteries and measure pressure differences across the valves.
Treatment Options
The treatment plan is determined by a council of Cardiology and Cardiovascular Surgery specialists, based on the patient’s symptoms, the severity of the valve disease (mild-moderate-severe), and heart function.
1. Medical Treatment and Follow-up
For mild and moderate diseases, medications are used to alleviate symptoms and protect the heart. Diuretics reduce edema, beta-blockers regulate rhythm, and blood thinners prevent clots. However, it should be noted that medications do not eliminate mechanical valve disease (calcification or tear); they only manage the process.
2. Heart Valve Repair (Valvuloplasty)
Today, the gold standard in surgery is to preserve the patient’s own valve if possible. Repair is preferred, especially for mitral valve and tricuspid valve insufficiencies. Its advantages include:
- Preserves the heart’s natural anatomy and function.
- Lower risk of infection.
- No lifelong need for high-dose blood thinners after surgery.
3. Heart Valve Replacement
In cases where the valve is too calcified or damaged to be repaired (especially in aortic stenosis), the valve is removed and replaced with an artificial valve. There are two types of prosthetic valves:
- Mechanical Valves: Made of carbon, very durable, and can last a lifetime. However, due to the risk of clot formation, patients must take blood thinners (warfarin/coumadin) for life and have regular blood tests (INR). They are preferred for younger patients.
- Biological Valves: Made from bovine or porcine pericardium. They do not require blood thinner use (except for the first 3 months). However, they have a lifespan of about 10-15 years and can wear out over time. They are preferred for elderly patients or those who cannot take blood thinners.
4. Non-Surgical Methods (TAVI and MitraClip)
With technological advancements, these procedures are performed without opening the chest cavity, by entering through the groin artery, for patients at high risk for open-heart surgery.
- TAVI (Transcatheter Aortic Valve Implantation): A procedure where a new biological valve is implanted into a narrowed aortic valve by entering through the femoral artery. It is life-saving, especially for elderly patients and those with high surgical risk.
- MitraClip: For mitral insufficiency, a clip is used to grasp the edges of the valve, reducing leakage, by entering through the groin.
Post-Surgery Recovery and Life
After open-heart surgery, patients are typically monitored in intensive care for 1-2 days and in the ward for 4-5 days. Bone healing takes approximately 6-8 weeks. During this period:
- Anticoagulant Use: Crucial for patients with mechanical valves. Medication dosages must be adjusted with regular INR tests.
- Infection Prevention (Endocarditis Prophylaxis): Patients with artificial valves or repair rings must use prophylactic antibiotics before dental extractions or surgical procedures. Infections in the body can settle on the valve.
- Regular Exercise: Walks performed under doctor’s supervision improve heart fitness.
Thanks to modern medicine, heart valve diseases are no longer a dreaded outcome. With early diagnosis, correct timing, and appropriate treatment, patients can return to their normal and healthy lives. If you experience chest pain, shortness of breath, or palpitations, consult a specialist physician without delay.
Video
Heart Valve Diseases – Expert Opinion
Most Frequently Asked Questions About Heart Valve Diseases
► Is heart valve disease dangerous?
Yes, because the disease can progress insidiously for a long time without being noticed. When valve function deteriorates, the heart muscle gradually thickens and loses its pumping power. If left untreated, it can lead to serious problems like heart failure.
► What is the recovery process like after surgery?
The patient is usually discharged within 1 week. Mild fatigue is normal in the first few days. Bone and tissue healing takes an average of 4-6 weeks. During this period, a return to normal life is achieved with regular walking, a balanced diet, and doctor’s check-ups.
► Who undergoes TAVI (Non-Surgical Valve Replacement)?
TAVI is a procedure to replace the aortic valve by entering through the femoral artery. It is a safe method generally preferred for elderly patients or those with co-morbidities who are at high risk for open-heart surgery.
► Can patients who have had valve surgery exercise?
Patients with mild valve disease or those who have completed their post-surgery recovery can engage in sports like walking and swimming with their doctor’s approval. However, strenuous activities like weightlifting or competitive sports that overexert the heart should be avoided.
Do You Have More Questions?
We have compiled the 25 most frequently asked questions and detailed answers from our patients about surgical risks, recovery process, TAVI method, and mechanical/biological valve selection on a special page.