Table of Contents
- What is Advanced Heart Failure?
- What Are the Causes of Reaching This Stage?
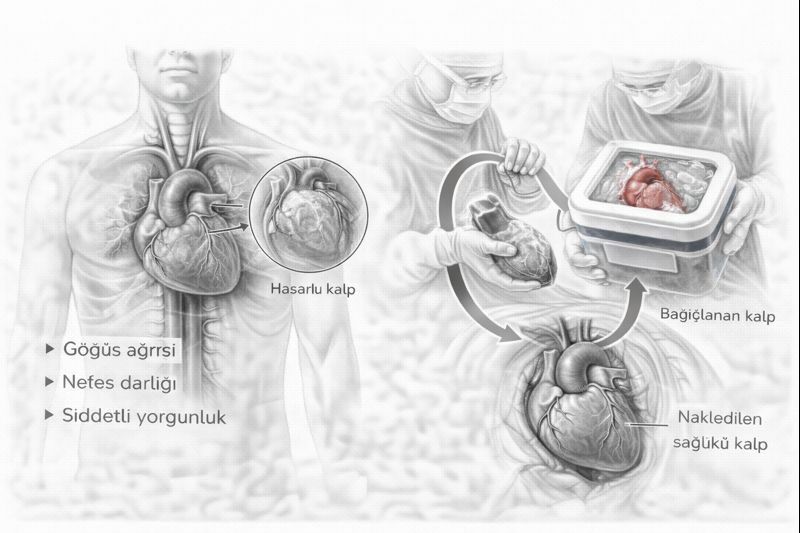
- Symptoms: The Body’s Call for Help
- Diagnosis and Evaluation Process
- Heart Transplantation: The Pinnacle of Surgical Treatment
- Mechanical Support Devices (LVAD): A Bridge to Transplant
- Medication Therapy and Palliative Care
- Conclusion
What is Advanced Heart Failure?
Advanced (or end-stage) heart failure results from damage to the heart’s structure or function that severely impairs its ability to pump enough blood to the body. These patients experience severe symptoms (shortness of breath, extreme fatigue) even at rest or with minimal exertion, despite optimal medication therapy, pacemakers (CRT), and other interventions. The disease is characterized by frequent hospitalizations, deterioration of organ function, and a high mortality rate. This condition indicates that the heart can no longer sustain its functions on its own.
What Are the Causes of Reaching This Stage?
Many chronic heart diseases can progress over time to end-stage heart failure:
- Ischemic Cardiomyopathy: Extensive damage to a large portion of the heart muscle due to previous widespread heart attacks is the most common cause.
- Dilated Cardiomyopathy: Weakening, enlargement, and loss of strength of the heart muscle due to genetic, viral, or unknown causes.
- Hypertrophic Cardiomyopathy: Abnormal thickening of the heart muscle, preventing the heart from filling with blood.
- Untreated Valvular Heart Diseases: Conditions such as severe aortic stenosis or mitral regurgitation placing excessive strain on the heart for years.
- Congenital Heart Diseases: Can develop over time in patients born with complex congenital anomalies who reach adulthood.
- Uncontrolled Hypertension: The heart becoming fatigued and failing after years of exposure to high blood pressure.
Symptoms: The Body’s Call for Help
In advanced heart failure, symptoms have completely taken over the patient’s daily life:
- Shortness of Breath at Rest: Difficulty breathing even when sitting or lying down, needing to increase the number of pillows at night.
- Extreme Fatigue and Cachexia: Even the simplest activities (dressing, walking) requiring too much energy to perform, significant muscle and weight loss.
- Widespread Fluid Accumulation in the Body (Anasarca): Significant edema in the legs, abdomen (ascites), and even the entire body.
- Loss of Appetite and Nausea: Occurs due to reduced blood flow to the intestines and edema.
- Decline in Cognitive Functions: Confusion or memory problems due to insufficient blood flow to the brain.
Diagnosis and Evaluation Process
Advanced heart failure is diagnosed based on the patient’s clinical condition and comprehensive tests. The evaluation process for heart transplantation or other advanced therapies requires a multidisciplinary approach:
- Echocardiography (ECHO): Evaluates the heart’s pumping strength (Ejection Fraction – EF), dimensions, and valve functions. EF is typically below 25%.
- Right Heart Catheterization: Directly measures intracardiac pressures and pulmonary artery pressure to objectively determine the severity of heart failure and pulmonary vascular resistance. This is a critical test for transplant suitability.
- Cardiopulmonary Exercise Test (CPET): Measures the patient’s maximum oxygen consumption capacity (VO2 max) to indicate functional status and disease prognosis.
- Blood Tests: Performed to evaluate kidney, liver, and other organ functions.
- Psychosocial Evaluation: Assesses whether the patient and their family are psychologically prepared for this challenging process and if their social support systems are adequate.
Heart Transplantation: The Pinnacle of Surgical Treatment
Heart transplantation is a life-saving operation for suitable advanced heart failure patients for whom no other treatment options remain. The goal is to offer the patient not only a longer life but also an active and high-quality life.
Who is a Candidate for Heart Transplantation?
The decision for transplantation is a complex process involving careful evaluation of many factors. General criteria for candidacy:
- Indication: Advanced heart failure symptoms and poor prognosis despite maximal treatment.
- Absence of Contraindications: Conditions such as active infection, recent cancer, irreversible severe lung, kidney, or liver damage, smoking/alcohol/substance addiction are contraindications for transplant.
- Age: Although 65-70 years is generally considered an upper limit, the patient’s biological age and overall health status are more important.
- Psychosocial Suitability: Having the psychological resilience and family support to adhere to the demanding post-operative treatment regimen.
Waiting List and Organ Matching
Eligible patients are registered with the National Organ Transplant Coordination System. The waiting list is determined by factors such as blood group compatibility, body size (donor and recipient should be approximately the same weight), tissue compatibility, and the patient’s urgency. This process is often very challenging for patients due to its uncertainty.
How is Heart Transplant Surgery Performed?
- Preparation and Access: When a suitable donor heart is found, the patient is immediately taken to surgery. The breastbone (sternum) is opened to access the heart.
- Cardiopulmonary Bypass: The patient is connected to a heart-lung machine that takes over blood circulation and respiration during surgery.
- Removal of the Diseased Heart: While the body’s blood circulation is maintained by the machine, the surgeon cuts and removes the patient’s own diseased heart from the main vessels (aorta, pulmonary artery, vena cavae).
- Implantation of the New Heart: The healthy donor heart, preserved in special solutions, is meticulously sewn to the recipient’s vascular ends.
- Starting the New Heart: After the sutures are completed, blood flow to the heart is restored. The new heart usually begins to beat on its own; sometimes a small electrical shock (defibrillation) may be required. Once heart functions are stabilized, the patient is weaned off the heart-lung machine.
- Closure: After bleeding control, the breastbone is closed, and the patient is transferred to intensive care.
Potential Risks and Complications
- Organ Rejection: The body’s immune system recognizes the new heart as foreign and attacks it. Lifelong immunosuppressive drugs are used to minimize this risk.
- Infection: Immunosuppressive drugs make the patient more vulnerable to infections.
- Drug Side Effects: Immunosuppressive drugs can lead to kidney failure, high blood pressure, diabetes, and an increased risk of cancer.
- Cardiac Allograft Vasculopathy (CAV): Narrowing of the coronary arteries of the transplanted heart over time is one of the most significant long-term problems.
Life After Transplant: A New Beginning
The post-transplant period requires careful, lifelong follow-up.
- Medication Discipline: Taking immunosuppressive drugs daily, on time, and at the correct dosage is vital.
- Biopsies and Check-ups: Heart biopsies and regular echocardiography check-ups are performed frequently in the first year to detect organ rejection early.
- Healthy Lifestyle: Protection from infections, healthy eating, regular exercise, and avoiding smoking are cornerstones of the new life.
Mechanical Support Devices (LVAD): A Bridge to Transplant
For some patients awaiting heart transplantation or those unsuitable for transplant, Left Ventricular Assist Devices (LVADs) can offer hope. These devices are mechanical pumps that take over the heart’s pumping function. They can be used as a “bridge to transplant” (to keep the patient alive until a suitable heart is found) or as “destination therapy” (to improve quality of life in patients without transplant options).
Medication Therapy and Palliative Care
For patients unsuitable for transplant or device therapy, treatment focuses on alleviating symptoms, improving quality of life, and reducing hospitalizations. Diuretics, vasodilators, and pain control are important parts of this process. The palliative care team helps support the patient and their family physically and spiritually during this challenging time.
Conclusion
Advanced heart failure is one of the most challenging areas of modern medicine. However, amidst this challenging outlook, heart transplant represents a new beginning for eligible patients. Despite requiring a difficult waiting period, complex surgery, and a lifelong treatment regimen, after a successful transplant, patients experience the joy of breathing again, walking, and spending quality time with their loved ones. The critical importance of organ donation in this process must not be overlooked; as every donation is a lifeline extended to a patient waiting with hope.